This essay was submitted to Open Philanthropy's Cause Exploration Prizes contest.
If you're seeing this in summer 2022, we'll be posting many submissions in a short period. If you want to stop seeing them so often, apply a filter for the appropriate tag!
Special thanks to Alex Hill for reading a draft!
Outline
Obstetric violence (OV) is usually defined as a negative experience, ranging from verbal abuse and neglect to physical abuse and non-consensual procedures, that a birthing person[1] experiences leading up to, during, or immediately following the delivery of a baby. While perpetrated by medical professionals or other staff at a birthing facility, OV has deep structural roots and complications. Examples and categories of OV can be found in Figure 1, provided for context.[2]
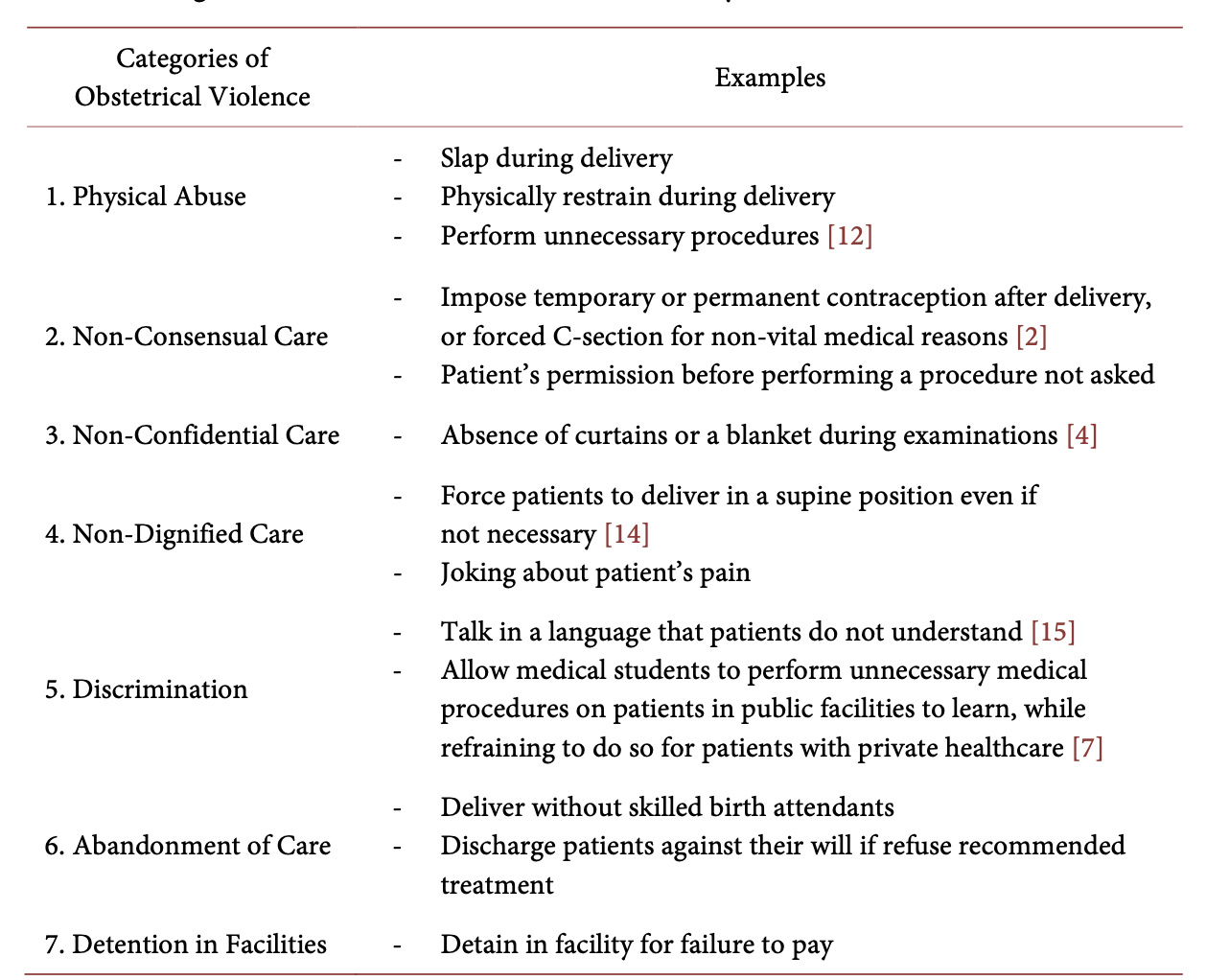
- I estimate that obstetric violence impacts ⅓ of births, or 46 million birthing people, worldwide.
- OV causes physical and psychological damage to the birthing person.
- OV reduces trust in the medical system that leads to lower utilization.
- OV is a soluble problem that requires the coordination of disparate parties to test and implement solutions like:
- access to birth rights education
- changing provider and hospital incentives and standards
- developing and expanding reporting mechanisms
- funding and supporting doulas and midwives
- giving birth plans more legal weight
Importance
Creating a human is a vulnerable experience that takes a physical and emotional toll on the birthing person even under ideal circumstances. Experiencing violence at a moment of extreme vulnerability negatively impacts both the birth outcome and the birthing person. Incidence of OV has been linked to higher rates of postpartum depression[3], anal sphincter injury, post-partum hemorrage, and infection.[4] Birthing people who experienced birth injuries or had secondary (non-elective) c-sections showed the highest severity of postpartum PTSD.[5]
Deliveries in which the birthing person experiences OV are correlated with higher rates of induction, episiotomy, and operative delivery (c-section).[6][7] The use of interventions like synthetic oxycontin or operative delivery disrupt processes that are critical to bonding and infant development such as skin-to-skin contact with the mother immediately after birth and breastfeeding.[8] Despite these tradeoffs, interventions to delivery can be medically necessary and consensual. The benefit of birthing in medical facilities under the supervision of skilled professionals is access to such interventions when needed. When these interventions are not medically necessary or consensual but occur anyway, that is classified as OV. In this scenario, the side effects of delivery interventions create avoidable pain and discomfort for the birthing person and place the health and development of the baby at risk.
The public health damage caused by OV is decreased trust in and utilization of healthcare services. Births attended by a skilled healthcare provider is an essential metric for the reduction of maternal and neonatal mortality.[9] Decreased trust in the medical system caused by OV may reduce skilled-birth attendance and thus contribute to increases in maternal/neonatal mortality.
Distrust in the medical system caused by OV has consequences beyond the scope of birth.
“OV can decrease willingness to seek medical care and trust in medical care, no matter if it concerns general medical care or childbirth related care. Therefore, OV was shown to have adverse consequences for women who experience it and the children of these women as well. These adverse consequences appear to persist over time and can intensify further the more time passes…”[10]
The delivery of a baby can serve as the ‘front door’ to healthcare, particularly in lower and middle income countries (LMICs). Birth presents the opportunity for a family or a community to establish a relationship with individual providers and the healthcare system more generally. Such relationships can lead to life-saving preventative care and the reduction of preventable mortality on a global public health scale. In the US, women make 80% of healthcare decisions for their families.[11] Even in countries where women have lower agency and purchasing power, women make the majority of healthcare decisions for themselves and their families.[12]
To further explore the possible reach of OV with a back-of-the-envelope calculation: if 50% of the estimated 46 million women who are victims of OV worldwide decided to reduce engagement or cease to engage with medicalized healthcare for themselves and their families (assuming 4 family members total), nearly 100 million people may miss critical care and increase disability-adjusted life years (DAYLS) as a result. While I think there’s validity in this line of reasoning (OV→ distrust → lower utilization → higher DAYLS), there is not enough data available on the worldwide rate of OV to confidently determine the full scope of impact.[13]
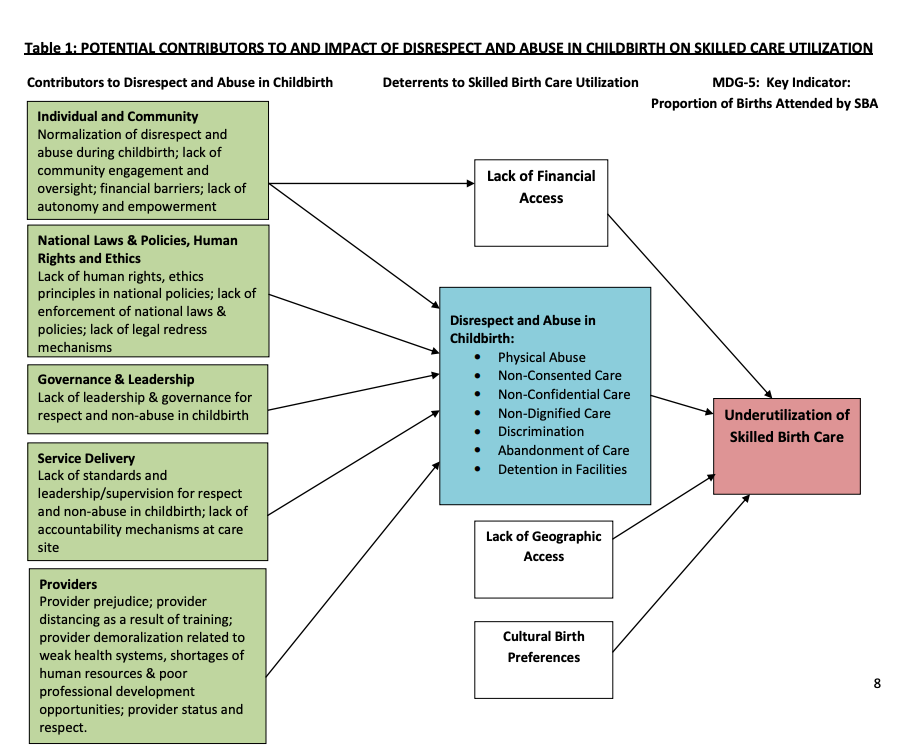
Eliminating OV has the potential to significantly impact human health and flourishing through reduction of suffering on the part of the birthing person and additional trust in the medical system that could lead to generations of increased vaccinations, preventative consultations, and screenings. Birth should be respected, encouraged, and protected as thus far the human race has no alternative method to support the propagation of our species.
Notes on the data
OV is a complex phenomenon that interacts with education level, race, and culture. Birthing people with the following characteristics are statistically more likely to experience OV: single, lower levels of literacy and education, lower socioeconomic status (SES), or part of a cultural or religious minority.[14] OV is not limited to LMIC - 17.3% of women in the US report experiencing OV.[15] The percentage increases to 28.1% when limited to a hospital setting. Women of color with a low SES in the US reported OV in 27.2% of cases, regardless of setting.
Studies comparing reported to observed outcomes have determined that birthing people under-report OV when surveyed themselves vs. when documented by an outside observer.[16] Because OV exists on a spectrum and in many cases has been normalized, birthing people may not be aware that the experience they have had is categorized as OV. In addition to awareness, accessible reporting channels may not exist or may not be safely and confidently accessible. Even if birthing people do recognize and have access to appropriate channels to report OV, normalization of negative birth experiences, stigma, and shame often hold them back from doing so. A literature review of OV published in the Open Journal of Obstetrics and Gynecology states, “the lack of consensus on what constitutes OV correlates with a dearth of screening tools, making it virtually impossible for women to take legal action, even for physically violent forms of [obstetric violence].”[17] Finally, the outcomes of studies conducted to observe and quantify OV are typically country-specific and not standardized across cultural differences and varying health systems.
The rates of OV vary significantly by region, survey method (observation vs. survey), and survey timing.
- A WHO-sponsored multi-country study (Ghana, Guinea, Myanmar, and Nigeria) published in 2019 determined that 42% of births observed by an informed observer included OV.[18]
- A 2016 survey conducted in Mexico found that 33% of people who had given birth within the last 5 years reported experiencing OV.[19]
- A 2021 study in Germany found that 76.3% of births surveyed included OV, the most prevalent category of violence reported being “lack of rapport between woman and provider.”[20]
- In France, 20% of births result in an episiotomy, 50% of which are unconsented.[21]
- A 2015 study in Ethiopia determined that 78% of birthing people experienced OV but only 21% reported experiencing OV[22], demonstrating the difference between self-report and observation as methods of estimating incidence.
- A 2020 study in Spain determined that 67.4% of birthing people surveyed experienced OV, 50% of which was physical violence.[23]
Taking into account the challenges in collecting and standardizing accounts of OV, the data we do have available indicates a significant number of women are subject to OV worldwide. I can say with 75% confidence that at least one-third of birthing people worldwide experience some level of OV. With ~140 million live births per year (a figure that does not include stillbirths or maternal mortality), that leads us to conclude that at least 46 million women per year experience one or more types of OV.
Neglectedness
From a policy perspective, Latin America has led the effort to protect women from OV. In 2007, Venezuela became the first country to define protection from OV as part of a woman’s right to lead a violence-free life. Mexico, Bolivia, Argentina, and Panama have subsequently codified women’s right to a life free from violence (obstetric and otherwise) into law.
While declarations and laws protecting the rights of birthing women express good intent, they have not delivered results. Mexico provides a case study in the failure of these laws alone to result in positive change. Following the national law, five Mexican states went above and beyond, modifying their penal codes to classify OV as a crime.[24] A recent study that sought to analyze “whether criminalising obstetric violence has been conducive to the recognition and observance of the reproductive rights of women” concluded that “incorporating obstetric violence under the criminal code has not led to a substantive difference in how the citizenship rights of pregnant and birthing women are recognised or observed.”[25] Furthermore, existing laws and statues are not usually invoked in the rare cases when OV is prosecuted. In Argentina, where statues exist prohibiting OV, “courts adjudicating tort suits continue to rely on a malpractice analysis rather than the norms of humanized childbirth and freedom from violence.[26] These examples demonstrate that codifying women’s right to a safe birth experience is not enough.
In 2014, the WHO issued a statement on “the prevention and elimination of disrespect and abuse during facility-based childbirth”[27] which mobilized some research and policy efforts. Paradoxically, the 2015 adoption of ‘reduction of maternal mortality to < 70 deaths per 100k live births’ as a UN 2030 Sustainable Development Goal (SDG) may have contributed to an increase in OV as some LMICs responded by over-medicalizing birth. While progress has been made in reducing the worldwide maternal mortality rate[28], the worldwide rate of c-sections has simultaneously increased to 21%, well above the WHO’s estimation of 10-15% medical necessity.[29] Some of the medically unnecessary c-sections performed are a symptom of OV while others may be direct examples of OV in situations where the birthing person did not consent to the operation.
As OV overlaps with violence against women and maternal/neonatal mortality, it is difficult to determine the percentage of money allocated to “child and maternal health” that specifically contributes to the reduction of OV. The lack of clarity and specification leads me to believe it is an underfunded sub-category. One example of funding specifically targeting OV is a clinic in rural Chiapas, Mexico opened and funded by Partners in Health that focuses on women-centered, humanized care under the supervision of midwives. With additional funding, this model could be analyzed and duplicated. Activist groups such as Improving Birth and Human Rights in Childbirth advocate for humanized, violence-free birth by educating pregnant people and supporting victims of OV.
One overlooked and underfunded aspect of OV reduction is the funding and incorporation into the broader medical system of midwives and doulas. The 2021 State of the World’s Midwifery report estimates a “global shortage of 900,000 midwives, which is particularly acute in low-income countries (LICs) and in Africa.” They conclude that “the shortage is projected to improve only slightly by 2030 unless additional investments are made.”[30] While the United Nation Population Fund, as part of their Maternal Health Thematic fund, is funding the training of midwives, to be a tool for OV prevention, midwives must be incorporated into the broader health system. Open Philanthropy can consider funding the training, certification, and incorporation of midwives and doulas into hospital settings to help offset this shortage.
Tractability
OV is a tractable problem that we have the real possibility of eliminating this century, given the resource allocation.
Many of the currently proposed solutions to OV err on the side of policy and legal solutions. A successful eradication of OV will need to include policy makers, lawyers, birth workers (doulas/midwives), OB-GYNs, hospital systems, and birthing people themselves. This significant coordination effort requires outside funding as each party comes to the table with their own incentives. While there may not be a single consensus-supported solution, the reduction and eventual elimination of OV, is not in itself a controversial goal.
I’ve outlined some interventions and included comments on the tractability, barriers, and dependencies between them.
Define the Problem
The first step in reducing OV is agreeing to a universal definition. Attempts have been made to categorize and standardize OV but studies conducted thus far do not leverage a universal definition. In the words of Drexel Law professor Elizabeth Kukura,, “there is no definition of obstetric violence that is universally adopted in global public health discourse or used consistently in the United States.[31]
Reporting incidents of OV and taking subsequent legal action require a clear definition. Additionally, a universal definition of OV will allow for more accurate research that can facilitate the prioritization of regions and tailor solutions to the most prevalent OV sub-categories. Open Philanthropy can allocate funding to the development of a worldwide scale to recognize and categorize OV. This intervention likely has high coordination costs. Pursued independently it won’t result in a significant reduction of OV, but it is essential to further research and may catalyze other OV interventions.
Educate Birthing People and Partners
Educating birthing people and those that they’ve chosen to support them (partners, friends, family) is an essential step in the elimination of OV. The ability to recognize violence begins with understanding your rights and the options available to you. A recent study in Spain found a positive correlation between attending childbirth education (CBE) and OV,[32] which implies that women who do not attend CBE may be experiencing OV and not recognizing it. Birth rights education, which may or may not be included in broader childbirth education (CBE), is not provided or accessible to all birthing people. Research on usage of and access to CBE is sparse. Women in higher income countries (HIC) who hire a doula may receive this type of education from them. Women who do not have access to CBE classes turn to family, friends, healthcare providers, and increasingly social media to understand and prepare for pregnancy and birth.[33]
Open Philanthropy can fund scalable, accessible, and reliable forms of CBE that include birth rights education and are able to reach more women worldwide. The development of culturally-specific, accessible clinical content with the potential for distribution via existing channels (apps, whatsapp, social media) can help women and their partners better understand OV and ways they can protect and advocate for themselves throughout pregnancy and birth. Existing digital health solutions targeting women in countries with high rates of OV can be funded and expanded to include birth rights education. This intervention is scalable, tractable and has the potential for significant returns if accompanied by changes to provider/hospital standards. No matter how informed and empowered birthing people are, without changing provider and hospital incentives, OV will still be a threat. At a minimum, those who receive birth rights education will be better prepared to recognize and defend themselves against it.
Build Accessible Reporting Mechanisms
Developing or expanding access and awareness to reporting channels through which birthing people, their companions, or other birth workers who have witnessed OV can file a formal complaint/investigation is critical to holding hospital systems and birthing facilities accountable. Assuring that such channels are safe to use and free from corruption will also be essential. Governments and/or NGOs will need to take on the role of developing, promoting, or maintaining such channels..
“Many would argue that it is impossible to effectively address maternal health care abuses without directly assessing the inequities in power between the maternal health provider and the woman giving birth.”[34]
Safe and useful reporting mechanisms are a good start to addressing power inequities. Outside funding like Open Philanthropy can accelerate the development of such reporting channels. The level of effort to implement or improve upon existing channels is likely high and would need to be country-specific, however this intervention could be initiated immediately and independently of other interventions listed. I’d consider this intervention to have a medium level of tractability, compared to the others considered.
Fund and Integrate Doulas and Midwives
There is a correlation between the involvement or presence of a doula or midwife and lower rates of OV. A birth doula is a non-clinical resource hired to guide and provide emotional support to women throughout pregnancy and birth. Doula-assisted births are less likely to experience birth complications and more likely to initiate breastfeeding.[35] A midwife is someone with clinical training who can safely deliver many low-risk pregnancies without additional clinical staff present.[36] I’ll group them together for the purpose of this discussion even though they do play separate roles.
Involvement of midwives and doulas may include education, delivery-room observers, a more holistic methodology, and the selection of an alternative birth setting. A midwife or doula is a knowledgeable third-party that is trained to recognize obstetric violence. There is no clear data on whether their presence alone reduces the rate of OV, but in general, delivery observers report higher levels of OV compared to the birthing person themself. Additionally, the involvement of a doula or midwife in HIC typically includes some CBE and the development of a birth plan, both of which are forms of education and preparation for the birthing person and their partner(s). Finally, doulas and midwives typically promote a person-centered approach to delivery sometimes called “humanized birth,” the goal of which is to respect the desires of the birthing person and cast them in the role of primary decision-maker. This methodology can sometimes be practiced in a birthing facility under medical supervision if facility rules and standards allow.
Because humanized birth opposes timelines, restrictions, and rules in favor of listening to the birthing person’s body, it is often easier to implement in private birthing centers or at home. Home births have a significantly lower rate of reported OV. For example, in the USA 28% of surveyed hospital births included OV and only 5% of home births.[37] In Mexico, those who were accompanied by a midwife outside of a hospital setting had a 2.8% rate of OV vs. 37.2% of those who gave birth in a public state hospital.[38] At the same time, in LMIC home births are associated with higher rates of maternal and neonatal mortality when unaccompained by a skilled birth worker.[39] Funding and supporting midwives may be a solution to simultaneously reducing OV and maternal and neonatal mortality.
A model of birth that is both respectful and efficient would maximize the knowledge and expertise of each available resource, having doulas and midwives play their respective roles in low-risk pregnancies while having fast access to informed, empathetic OB-GYNs and operating rooms. Collaboration and respect between all parties (birthing person, doula, midwife, OB-GYN and any other hospital staff) is essential. However, there is often tension between traditional (community midwives, doulas, etc.) and medicalized healthcare. Stemming from a lack of respect for midwifery, “long-standing professional turf battles between physicians and midwives have limited access to low-cost, low-intervention midwifery care for many women.”[40] Many hospitals and birthing facilities explicitly ban doulas from supporting births or effectively ban them by limiting the birthing person to choosing a single companion. This trend has been exacerbated by additional limitations on attendance put in place by hospitals during COVID-19.[41]
The opportunity to experiment with models for resolving this tension between more traditional methods and modern medicine is challenging politically and legally. A funder like Open Philanthropy could invest in existing pilots that promote humanized birth and collaboration between clinicians and other birth workers, measure the rate of OV, and share best practices for expanding and duplicating the model. One example is a J&J foundation pilot in Mexico that trained midwives and placed them in public hospitals. Additionally, as noted previously, Open Philanthropy can help address the shortage of midwives by funding training, support, promotion, and access to their services. I believe this intervention has the highest tractability of those outlined.
Change Incentives and Improve Conditions for Providers
To achieve widespread structural change, providers and hospital systems, the perpetrators of OV, must be included in the solution. In a hospital where there are limited beds and the doctor is reimbursed per birth, doctors are incentivized to optimize for speed over respecting the preferences of the birthing person or the timelines dictated by the baby.
It is common for hospital systems to have standards that prevent or limit outside observers from entering a delivery room, be operating over-capacity which can result in neglect or lack of privacy, or dictate the amount of time for and/or which physical positions are permitted for labor in the hospital. Additionally, overworked and underpaid staff are factors that correlate with higher rates of OV.[42] Through these standards, hospital systems set providers up for failure.
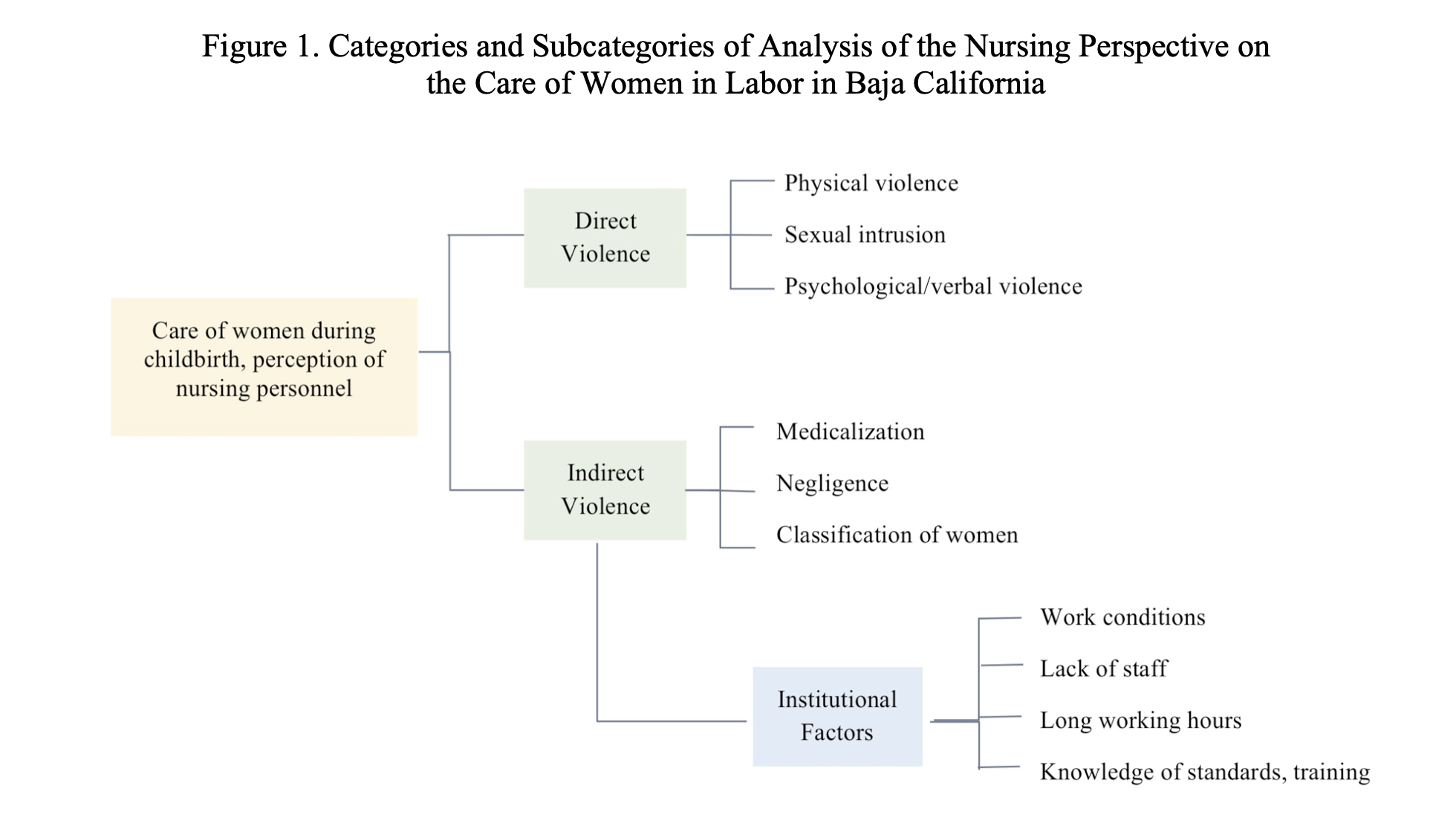
Providers are often incentivized against carrying out humanized birth practices by liability risk factors. As a post on the Harvard Law forum states, “when compared to the limited liability risks associated with violating a birthing woman’s autonomous choices, it is clear that providers wishing to minimize legal risk are acting rationally when they prioritize fetal interests over maternal interests.”[44]
Clinical professionals involved in the birth process, from OB-GYNs to nurses to general practitioners also need to be well-versed in recognizing OV, the consequences, and the alternatives such as humanized birth.[45] Finally, providers need to be supported with adequate resources to provide pain relief and comfort to birthing people.
Changing the operating conditions and incentives of hospital systems is arguably the least tractable OV intervention but also the one that most directly addresses the root cause of OV. Building independent birthing facilities where resources and labor conditions can be controlled is one admittedly costly option. An outside funder can support grassroots efforts advocating for better working conditions in public hospitals, fund OV training for clinicians, and fund solutions addressing worsening clinical labor shortages.
Formalize Birth Plans
A birth plan is a seemingly innocuous but sometimes controversial tool that helps birthing people think through their options, preferences, and prepare for various delivery scenarios. The information contained in a birth plan can range from preferences (“I would like to play my own music in the delivery room”) to medical requests (“no episiotomy” or “perform newborn exams in the room with me”). A pregnant person may develop a birth plan independently, in coordination with a doula or midwife, or in collaboration with their OB-GYN.
Depending on the facility at which the delivery occurs, a birth plan may or may not be taken into account at all. A birth plan can also be helpful in the selection of a facility, if the birthing person has the means and geographic access to a variety of choices. Research has shown that birth plans are a valuable communication tool regardless of the extent to which they are adhered to in the end.[46]
An idea has been proposed in the legal community to treat birth plans similarly to advance directives. Advanced directives are legally-recognized documents used to inform providers and family of one’s medical preferences in the event that the individual is not able to express these preferences themselves. They are commonly used for end-of-life care. Medical professionals are not forced to comply with advanced directives but are bound to redirect care to a provider who is able to comply.
Open Philanthropy could fund research and partner with governments and/or hospital systems to trial the idea of stricted birth plan adherence. Pursuing such an effort, considering the expected hesitancy and resistance from the medical community, requires the scale of funding that an outside organization like Open Philanthropy would be able to support. I consider this intervention to have low tractability due to the need for legislative action.
Conclusion
OV is an important problem with some tractable solutions. It is relatively neglected as a sub-category of maternal and child health. Additional research that defines and confirms thel levels and severity of various types of OV will be essential in making intelligent progress toward solutions. The intersections with broader gender-based violence and the reliance on changing hospital systems and taking legislative action are significant barriers that should be considered when allocating funding.
Areas of Further Research
Open questions or areas of further research that I have identified include:
- Is elimination of obstetric violence too broad a goal? Should focus be placed on reduction of medically unnecessary/non-consensual c-sections, for example.
- Country-specific policies and instruments that specifically protect doctors or incentivize them to prioritize fetal health over the birthing person’s preferences
- Areas of overlap in the interventions between maternal/neonatal mortality and maternal morbidity and OV.
- More in-depth calculation on the DALYS of OV
- Along with developing a universal definition, it would help to silo OV by type/level of violence and prioritize the pursuit of interventions accordingly.
- The use of OV as a tool for political violence (e.g. the forced sterilization of indigenous women in Peru in the late 1990s) is also important but falls outside the scope of this specific investigation.
- There is significant overlap between obstetric violence and gender-based violence more broadly. Addressing OV in regions with high rates of GBV may be difficult or impossible.
Limitations and Disclaimers
- I’m not a subject matter expert, nor am I a doctor, lawyer, researcher, or public health official. I welcome feedback from anyone, particularly those who are subject matter experts.
- My research and examples are skewed toward Latin America because that’s where I am based.

I sincerely hope this cause will be taken as seriously as possible and thoroughly examined.
On an anecdotal basis, I have been repeatedly surprised just how many people around me have had significant experiences along these lines. I would never have guessed this before my friends all were in child-bearing age.
I also think the relevance of this cause area might typically remain hidden from public sight because:
We should also naturally be open to the idea that OV happens much more frequently than assumed given that