TLDR
Vida Plena is a nonprofit organization that is tackling Ecuador's mental health crisis through cost-effective, proven group therapy led by local leaders from within vulnerable communities. We do this through the direct implementation of Group Interpersonal Therapy, which is the WHO's recommended intervention for depression. We are the first to implement it in Latin America.
We launched in early 2022 (see our introductory EA forum post) and took part in the Charity Entrepreneurship Incubator program that same year. In the fall of 2022, we carried out a proof concept alongside Columbia University, which found positive results (see our internal report, and the report from the Columbia University Global Mental Health Lab).
So far this year, we've made a positive impact on the lives of 500 individuals, consistently showing significant improvements in both depression and anxiety. Our strategic partnerships with local institutions are flourishing, laying the groundwork for our ambitious goal of scaling our reach to treat 2,000 people in 2024.
For this marginal funding proposal, we seek $200,000 to expand our work and conduct research to apply behavioral science insights to further depression treatment in Latin America. This enhanced therapy model will be evaluated through rapid impact assessments, deepening the evidence base for our work, and culminating in a white paper and a RCT in 2025. We also share additional ways to support our work.
This post was written by Joy Bittner and Anita Kaslin, Vida Plena’s co-founders. In it, we share:
- An overview of Vida Plena and our work
- The scope and scale of the problem we are addressing
- Our solution and the evidence base
- Our initial results to date
- Present our proposal for marginal funding opportunities
- Additional funding opportunities and how you can support our work

1) An Overview of Vida Plena and Our Work
Problem:
Mental health disorders are a burgeoning global public health challenge and disproportionately affect the poor. Low- and middle-income countries (LMICs) bear 80 % of the mental health disease burden. Mental illness and substance abuse disorders are significant contributors to the disease burden, constituting 8.8% and 16.6% of the total burden of disease in low-income and lower-middle-income countries. According to The Wellcome Global Monitor on Mental Health, the largest survey of depression and anxiety rates worldwide, Latin America exhibits the highest rates globally.
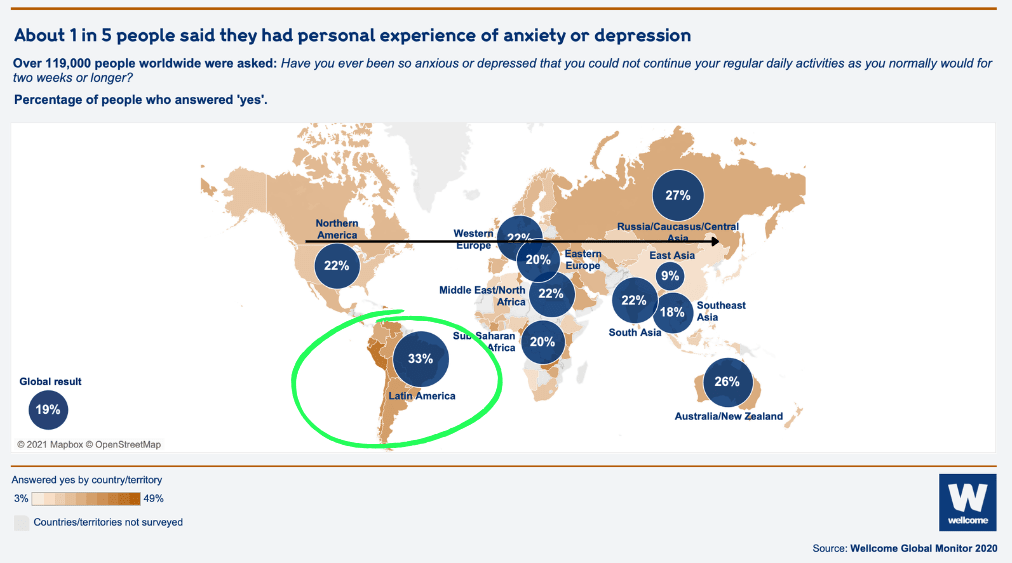
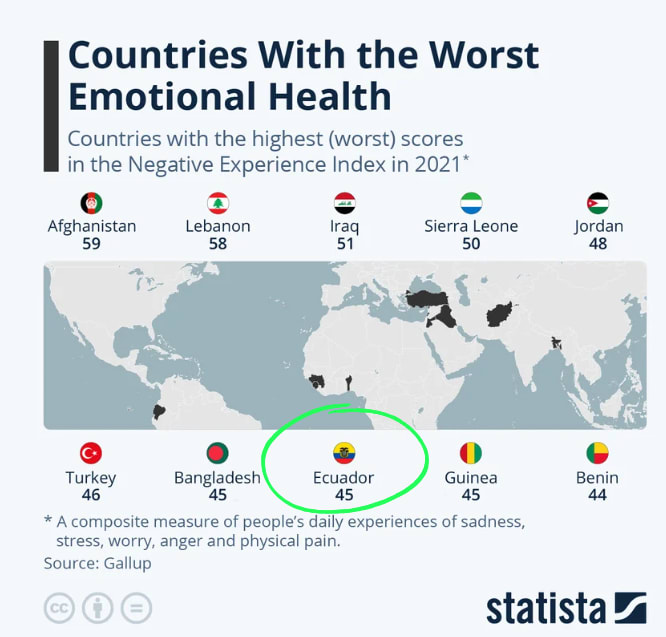
This situation is worsened by low public investment. Despite a 2021 Gallup poll ranking Ecuador among the top 10 worst countries in the world for emotional health, only 0.04% of the national healthcare budget is dedicated to mental health - 9x less than other Latin American countries. Therefore, most mental health conditions, especially depression, go untreated.
Depression is defined by intense feelings of hopelessness and despair. The result is suffering in all areas of life: physical, social, and professional. Untreated depression's repercussions extend to daily economic and life decisions, impairing attention, memory, and cognitive flexibility. This hampers personal agency and worsens the cycle of poverty and mental disorders. Poor mental health is associated with a host of other issues: chronic medical conditions, drug abuse, lower educational achievement, lower life expectancy, and exclusion from social and professional arenas. As a result, it's not surprising that health problems are related to economic factors such as loss of productivity, absenteeism (both for the patients and caregivers), and financial strain due to the cost of care.
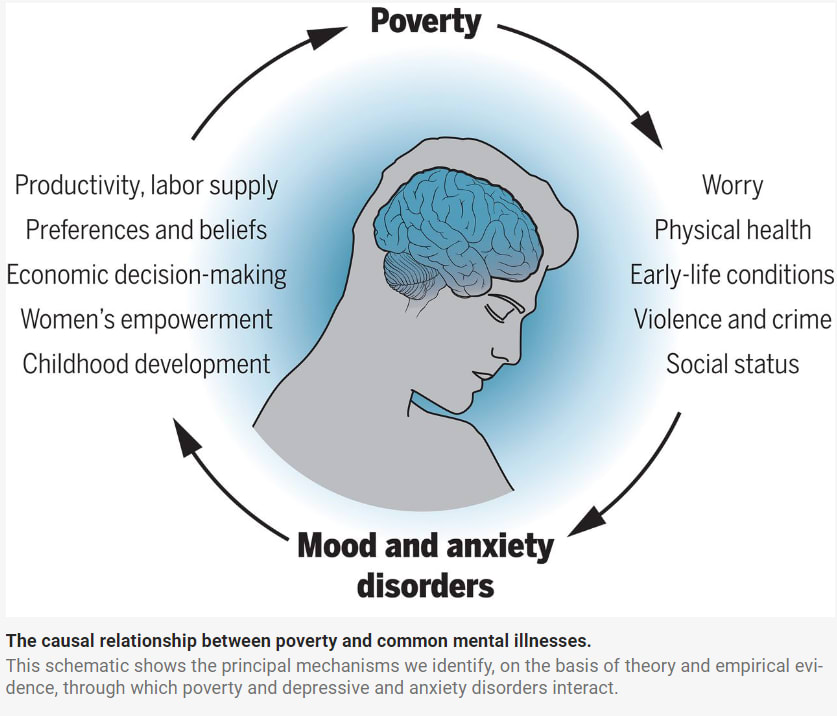
Conversely, research underscores the link between positive mental health and agency. Enhanced mental well-being fosters resilience and emotional regulation, empowering individuals to navigate challenges, set goals, and make value-aligned choices.
Our Solution & Theory of Change:
Vida Plena provides cost-effective depression treatment in vulnerable communities using a model known as group Interpersonal Therapy (g-IPT), which the WHO recommends as a first-line treatment for depression in low-income settings. A 2006 RCT found that g-IPT yields lasting depression reductions in 75% of participants. Furthermore, providing care through community facilitators is a proven cost-effective scaling solution. By training community members to provide g-IPT, Vida Plena seeks to improve wellbeing, life satisfaction, and personal agency among individuals struggling with depression.

The g-IPT intervention consists of 8 weekly group therapy sessions with 6-8 participants. These sessions equip participants with skills to manage depression, nurturing agency, and self-confidence. Weekly data monitoring yields promising results: 71% of Vida Plena participants show significant symptom improvements. Furthermore, Vida Plena is testing a WhatsApp service via the Turn.io Chat for Impact Accelerator, potentially enhancing participant outcomes.

A key component of g-IPT involves training local community members as group facilitators, enhancing cost-effectiveness and scalability. This method is shown to be effective in Uganda by Bolton et al. (2003) and corroborated by Bass et al. (2006). They found that community-led g-IPT significantly reduced depression as compared to a control group. This resulted in an absolute reduction of depression symptoms in 75% of participants 6 months following the conclusion of treatment. In Vida Plena’s own work, similar improvements have been observed in pre- and post-treatment assessments, with 71% of participants reporting clinically significant reductions in symptoms. While Vida Plena’s programs last 8 weeks, short-term therapies are effective; showing long-term positive effects even after five years (Baht. et al 2022).

Who We Impact
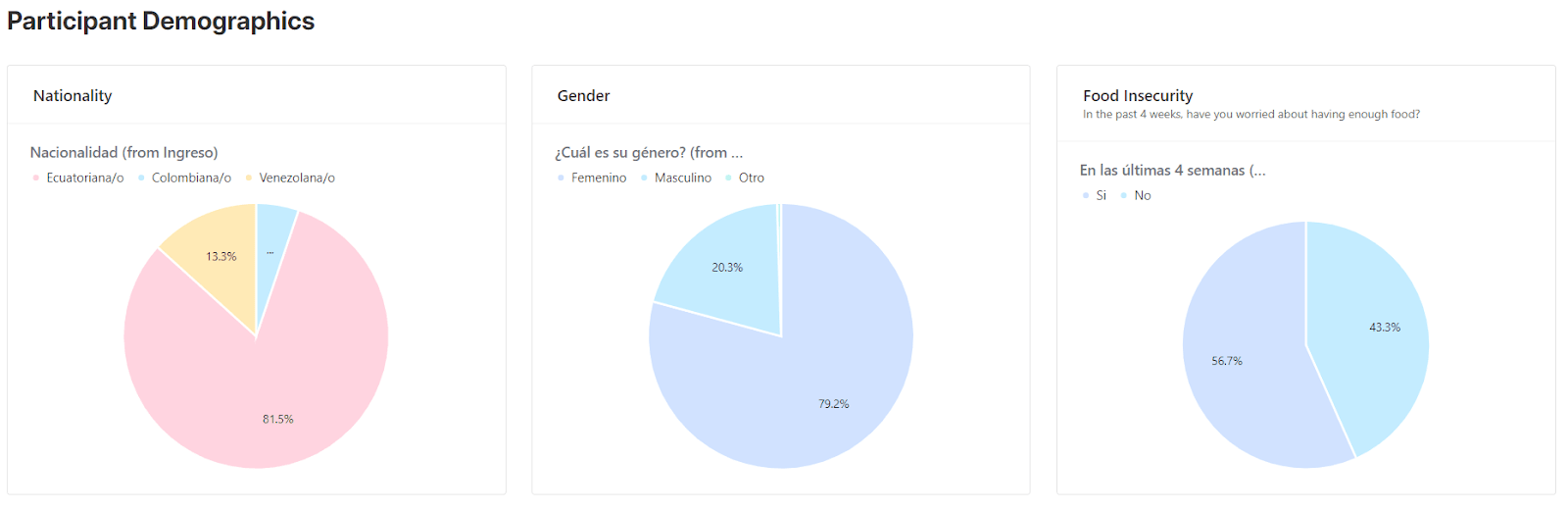
Vida Plena works with both men and women who are experiencing depression, specifically focusing on marginalized and low-income communities in Ecuador.
Within this general demographic, we also work with several highly vulnerable populations, including elderly adults, incarcerated women, refugees, and forced migrants, individuals in residential addiction treatment centers, families of trafficking victims, and victims of gender-based violence.
By collaborating with partner NGOs and government entities, we actively identify those in need of support. An essential aspect of this project will be the development of customized messaging and programs tailored to address the specific needs of these distinct subpopulations.
Our Team and Our Partners
Joy Bittner brings to her role as CEO 15+ years of experience leading social ventures in LATAM. Clinical Supervisor Anita Kaslin, an Ecuadorian psychologist, has over a decade of experience caring for marginalized groups with local cultural competence.
Additionally, our 11 facilitators live in the communities where they work.
Vida Plena’s model aims to come alongside other organizations and thus deepen the effectiveness of both programs by pairing mental health with other types of social service interventions.
In just our first year we have gained recognition and established partnerships across all sectors in Ecuador: public, private, and non-profit. For example, we are partnering with USAID and IMPAQTO, a start-up accelerator and social business incubator, to provide mental health services to women entrepreneurs. We are working with the public sector through the Quito Department of Health. We also work with a variety of international and local NGOs, including World Vision, and Jesuit Refugee Services.
Results to Date
Vida Plena was launched in 2022 and took part in the Charity Entrepreneurship Incubator program that same year. In the fall of 2022, we were certified in g-IPT by Columbia University and carried out a proof concept, which found positive results (see our internal report, and the report from the Columbia University Global Mental Health Lab).

So far in 2023, we have reached 483 participants, achieving the following outcomes:
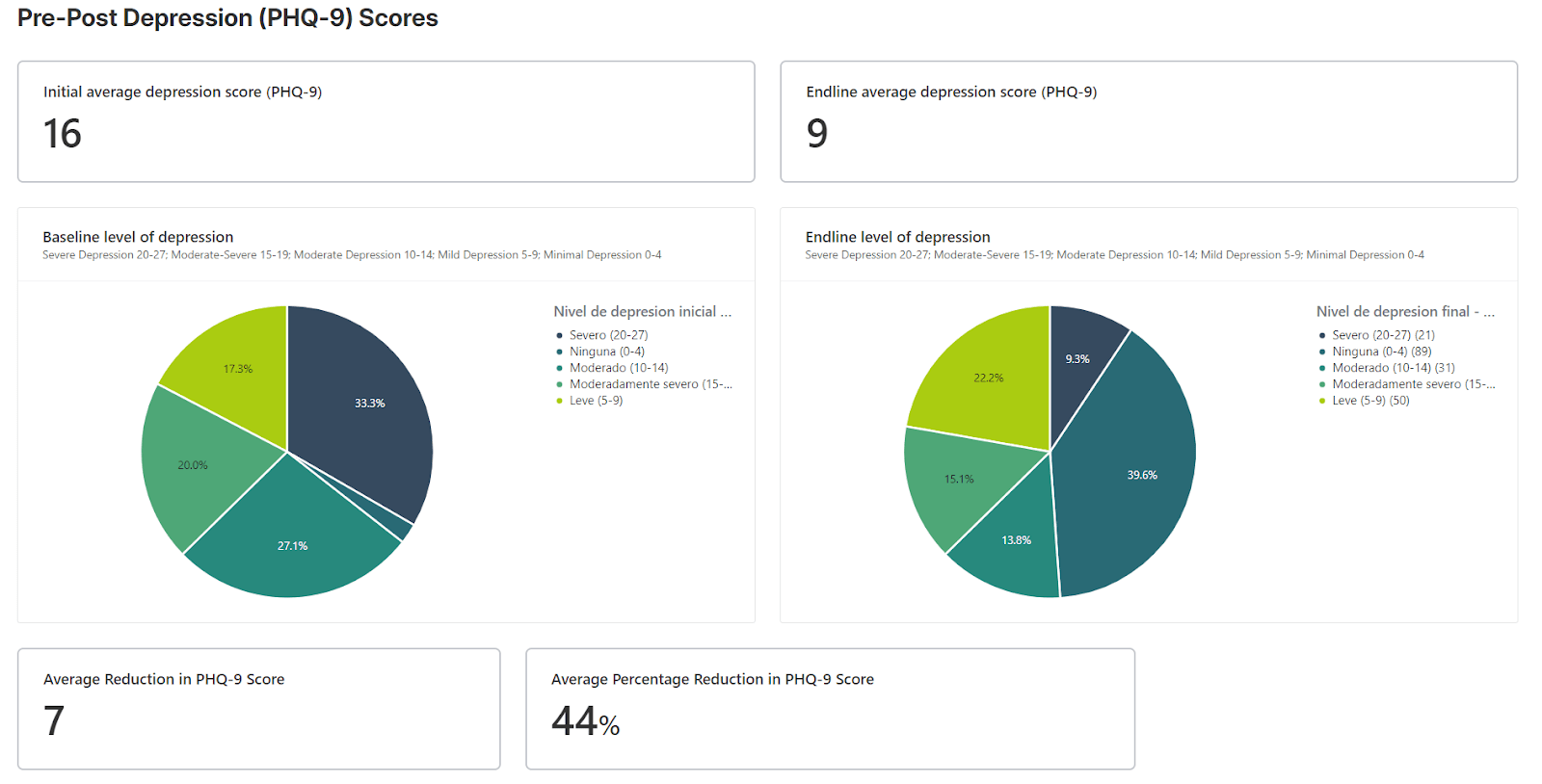
Moreover, we have cultivated partnerships with a variety of local organizations within Ecuador, spanning the social, private, and public sectors. Our collaborators include
- NGOs such as World Vision and FUDELA
- Private companies that employ minimum-wage workers, such as the delivery service Rappi and a local grocery chain, Santa Maria
- National universities
- Government institutions, such as a women's prison, and a Ministry of Health addiction treatment program.
Our partnership model amplifies the benefits of good mental health and enhances the overall impact of their programs.
Estimated Cost Effectiveness
Once operating fully at scale, we estimate that it will cost Vida Plena $462 to prevent one DALY.
However, we prefer measuring impact in well-being-adjusted life years (WELLBY), which gauges overall wellbeing, in contrast to DALYs’ focus on disease and disability. Using this metric, we estimate it costs $17 to enhance a person’s well-being by one WELLBY, making it 8x more cost-effective than the benchmark of direct cash transfers.
If we can meet our 2024 funding goals, we will scale the program and reduce the current cost of $216 per participant closer to the 2024 target of $120 per participant. We expect that this will lead to clinically significant improvements in depression symptoms in 75% of participants.
Note: We created these projections by extrapolating from the CEAs of other organizations using g-IPT, taking into account Vida Plena's projected expenses, the average Ecuadorian household size for spillover effects, the counterfactual treatment gap, and the likelihood of success. For more details about our expected cost-effectiveness at scale, see this forum post.
Roadmap for 2024 and Beyond

In 2024, Vida Plena is set to extend mental health treatment to 2,000 individuals by incorporating 20 new community facilitators into our dedicated team. An innovative step forward includes piloting a partnership model with private businesses, ensuring their employees have access to vital mental health care through paid collaborations. Our ultimate aim is to reach every corner of Ecuador, particularly in regions currently devoid of such services. We actively seek partnerships with both local and national government entities, aspiring to become essential service partners. Looking ahead, our three-year plan includes the ambitious goal of expanding our impact beyond borders and initiating projects in neighboring countries like Colombia.
2) Marginal Funding Proposal: Enhancing g-IPT via Behavioral Science
The core of this marginal funding project proposal is to continue iterating and improving the most cost-efficient version of g-IPT for scaling throughout Latin America. We expect the current g-IPT model can be improved by integrating behavioral science. Vida Plena aims to enhance engagement and deepen long-term outcomes by employing rapid learning cycles that apply expert insights from behavior design specialists and academic collaborators.
This project's output will be a comprehensive white paper, detailing findings and processes for improved depression outcomes. Additionally, we aim to build organizational capacity for a large-scale randomized control trial in 2025. With this evidence base, Vida Plena aspires to broad adoption and funding of g-IPT through governmental scaling support.
Total project funding needed: $202,400
see the project Budget for further details
Main Project Objectives
- Objective 1: Identify behavior science techniques and tools to improve participant enrollment and engagement. This will include the completion of the following steps:
- Behavior Analysis: Analyze the current enrollment and engagement patterns. Identify bottlenecks or points where participants drop off or disengage.
- Conduct a literature review and consult with experts to identify the most appropriate behavior-driven strategies such as personalization, gamification, social norms, reducing friction, timely reminders, etc.
- Objective 2: Rigorously test and evaluate identified techniques and tools to see which leads to better participant outcomes. Outcome improvements will be measured by:
- Tracking overall enrollment and per-session attendance to identify potential drop-off points.
- Pre- post-assessments; 3 and 6-month follow-up assessments: Collect data on depression symptoms (PHQ-9), anxiety (GAD-7), post-traumatic stress (PCL-5), subjective well-being, and other relevant indicators before and after the g-IPT treatment to assess how modification of the program using behavior science insights impact these measures. If successful, we will expect to see improvements better than the current baseline measures.
- Participant and therapist qualitative feedback: Gather feedback through surveys, interviews, and focus groups to understand the effectiveness of the modified g-IPT model and gather suggestions for improvement.
- Objective 3: Incorporate the most effective behavioral science techniques to create an enhanced version of g-IPT
- Timely completion of the white paper documenting project findings including a thorough analysis and clear presentation of insights from behavioral science integration.
- Discussion of scaling implications, presenting challenges and opportunities, and a cost-effectiveness analysis of various interventions
- Evaluation through peer review and expert feedback on quality and implications for scaling up g-IPT.
- Objective 4: Develop organizational capacity for Vida Plena to carry out an RCT in 2025. Success will be shown through:
- Development of Replicable Internal Workflows: Develop clear workflows and processes for different stages of the RCT, from participant recruitment and randomization to data collection and analysis. Ensure that everyone understands their roles and responsibilities.
- Data Management Plan: Develop a robust data management plan that includes data collection tools, data storage protocols, and data quality assurance processes.
- Ensure sufficient participant enrollment: Aiming for a robust sample size to ensure statistically significant results, we will collaborate with academic partners to determine the requisite number of participants.

Primary Risks to Project Success or Potential Setbacks
1. Insufficient data collection: If the project team does a poor job with data collection, it may hinder the ability to draw meaningful conclusions from the study. To address this issue, the project plans to hire a Monitoring and Evaluation (M&E) expert who will oversee data collection and monitoring processes, ensuring the accuracy and completeness of data. We will also consult with academic partners.
2. Inadequate participant enrollment: The inability to enroll enough participants for comparison groups could limit the project's statistical power and validity. To mitigate this risk, the project will employ an outreach specialist to establish partnerships with local institutions, enhancing participant recruitment efforts.
3. Misapplication of behavioral science strategies: Failure to apply the principles of behavioral science correctly may lead to ineffective interventions and outcomes. To avoid this, the project will collaborate with area experts and academics, ensuring the appropriate design and implementation of behavioral science strategies.
3) Additional Funding Opportunites:
In addition to the "Enhancing g-IPT via Behavioral Science" proposal described above, there are several other ways that Vida Plena could benefit from additional, marginal funding:
- $120 - Individual Support:
- Provide comprehensive treatment for one person, covering 9 sessions and ongoing follow-ups.
- $800 Monthly / $9,600 Annually - Group Facilitator:
- Hiring an additional Community Facilitator will extend care to approximately 400 more individuals, ensuring continued support.
- $50,000 - Expansion to New Region:
- Facilitate our expansion into a new region in Ecuador. This includes the establishment of training and outreach teams, bringing vital mental health care to areas currently underserved and neglected, beyond our current operations in Quito.
Possible Reasons for Not Funding Vida Plena:
- Impact Uncertainty: Our cost-effectiveness figures are projections, lacking local data for a control group (we aim to carry one out in 2025). Although our program's effectiveness is backed by other organizations' RCTs, results come with inherent uncertainties. Additionally, some readers might prefer DALYs over WELLBYs for cost comparisons, and therefore other initiatives will be more cost-effective.
- Government Adoption Challenges: The big-picture scaling plan is to have g-IPT adopted into the national healthcare system. While we are making progress with local entities, national government implementation isn't guaranteed. Still, we believe direct implementation could still be a cost-effective option, especially with diverse funding sources.
Reasons to Fund Vida Plena:
- Sole EA Health Organization in Latin America: Funding us provides an opportunity to build local credibility and establish a significant foothold in the region.
- Contribution to Treatment Models: Your funding would contribute to expanding the evidence base for improved treatment models. This not only benefits participants in our programs but also aids thousands globally relying on group interpersonal therapy (g-IPT) programs.
- Path to Self-Sustainability: Vida Plena is actively moving towards self-sustainability. We are developing a co-payer model with local businesses and securing contracts with development agencies. Strengthening our credibility with these entities reduces dependency on private donations in the future.
- Advocacy for Mental Health: If you care deeply about mental health and have witnessed the impacts of negative mental well-being, supporting Vida Plena means contributing to the positive mental health experiences of others.
How You Can Help:
Donate:
- If you'd like to support us, consider donating on our website. Donations are tax-deductible for US residents. For bigger contributions, let's chat! Drop an email to joy@vidaplena
Tell a Friend:
- Know someone who'd be interested? Share our story! Whether it's this post, our website link, or encouraging them to join our newsletter, your recommendation matters.
Stay in Touch:
- Want to keep up with our work? Follow us on LinkedIn, Instagram, or subscribe to our newsletter.
Thanks for being part of our journey! Got questions or curious about funding for organizations like ours? Leave a comment, and we'll get back to you.


Thanks for the update, Joy and Anita. Great work! In terms of expansion into a new region, what factors would determine the optimal timeline on that? Is it some tradeoff between the fixed costs of starting a second project vs the marginal cost of outreach being lower in a new area (low-hanging fruit)? Or more to do with demonstrating the impact in different types of communities in order to attract investment from the national government? I suspect the marginal costs might actually stay lower in Quito for quite some time due to local word of mouth. Best wishes to you in 2024, I am excited to see how this develops.
Hi Mike, thanks so much for all your support and these thoughtful points.
Yes, there are additional costs associated with geographic expansion, and we believe these costs are justified for several reasons:
Testing Demand and Adaptation: By expanding to more rural locations, we aim to assess the demand for and adaptability of our services. Urban life in Quito is fast-paced, and we've noticed various factors competing for people's attention, making it challenging for group attendance. Most other g-IPT programs operate in rural settings, where individuals may have more time. This expansion allows us to explore whether there are better rates of treatment adherence, with participants completing all eight sessions.
Building a Demonstration Case: As you suggested, this expansion helps us build a demonstration case, primarily for provincial and local governments. Regional government staff are generally more accessible than national government officials, and showcasing the value of providing mental health care can influence policies at these levels (hopefully leading to national government adoption)
Higher Counterfactual Value: In general, the counterfactual value of providing mental health care is higher in third-tier cities and rural communities due to the concentration of government services in larger cities. If we can effectively manage costs and prevent an overall increase, we believe there is a moral imperative to extend support to those with fewer alternatives.
thank you so much again and welcome further questions and feedback!
Inspiring work, the prospect of enhanced g-IPT is especially encouraging as that could further boost cost-effectiveness for mental health interventions generally. Looking forward to the next update - mucho suerte!
Thank you so much, Philippe! Yes, we are excited about the possibilities of combining insights from different fields and seeing what the date shows us.